About Us

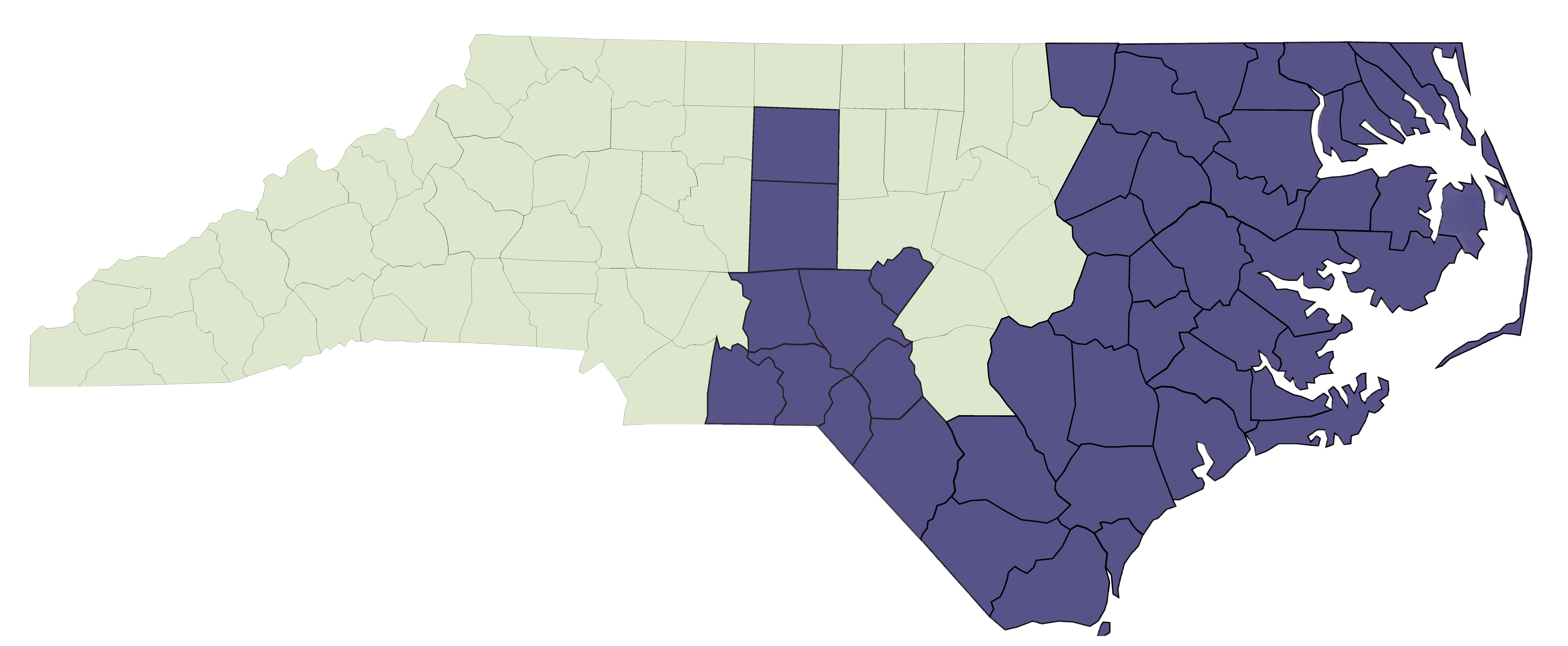
Trillium Health Resources is a Tailored Plan and Managed Care Organization (MCO) that manages serious mental health, substance use, traumatic brain injury, and intellectual/developmental disability services in North Carolina. For individuals receiving Medicaid through the Tailored Plan, we cover physical health care and pharmacy services as well. We cover the following counties: Anson, Beaufort, Bertie, Bladen, Brunswick, Camden, Carteret, Chowan, Columbus, Craven, Currituck, Dare, Duplin, Edgecombe, Gates, Greene, Guilford, Halifax, Hertford, Hoke, Hyde, Jones, Lee, Lenoir, Martin, Montgomery, Moore, Nash, New Hanover, Northampton, Onslow, Pamlico, Pasquotank, Pender, Perquimans, Pitt, Randolph, Richmond, Robeson, Sampson, Scotland, Tyrrell, Warren, Washington, Wayne, Wilson.
Trillium takes an innovative approach to health care. We invest in technology that drives independence and builds connection for those with developmental disabilities. We support our rural areas and improve ways our communities can access health services. We find unique solutions to integrated health care, contributing to training tools for providers serving those with serious mental health and substance use needs. We have experience with the needs of the individuals and communities we serve. We deliver the right services, in the right amount, at the right time. We know our region and the people who live in our counties. We know how to treat, support, and serve them most effectively
We work with our provider network to strengthen foundations of well-being and help deepen connections between citizens and their communities. Together with our state leaders, we are invested in the future of the public health system to help everyone in our region.
Our communities are only as strong as their people. Well-being needs a sturdy foundation at the start to prevent issues later and keep it standing through all kinds of weather. Our number one focus is helping every person we serve get the services needed to improve well-being and live a fulfilling life. We’re invested in every one of you.
Mission & Vision
Mission
Transforming lives and building community well-being through partnership and proven solutions.
Vision
For every community and individual we serve to reach their fullest potential.
Trillium manages services for:
- Medicaid members placed on the Trillium Tailored Plan.
- Medicaid members placed in NC Medicaid Direct.
- People without insurance or who are underinsured with state-funded behavioral health services.
- The NC Innovations Waiver (1915c Medicaid Home and Community-Based Services)
- Non-medical services such as supported employment.
In addition, we receive local dollars (from counties, etc.) for prevention, training on mental health, and wellness.
Complaints & Grievances
We welcome your feedback, both good and bad. Knowing about problems helps us make improvements. Hearing about good experiences gives us important information about our providers. Please call Member and Recipient Services at 1-877-685-2415 let us know about any issues with your care, or you can visit our Complaint | Grievance form to file a complaint.
Complaint | Grievance formTrillium Office Locations
Headquarters
Headquarters
201 West 1st Street
Greenville, NC 27858
Regional Offices
Please make arrangements ahead of time with Trillium staff to ensure someone is available to meet you if you need to visit a Trillium office.
Regional Offices
3809 Shipyard Blvd.
Wilmington, NC 28403
144 Community College Road
Ahoskie, NC 27910
514 East Main Street
Beulaville, NC 28518
302 Tarboro Street W.
Wilson, NC 27893
1100 Seven Lakes Dr,
West End, NC 27376
938 New Century Drive
Asheboro, NC 27205
3802 Robert Porcher Way
Greensboro, NC 27410
307 N. Main Street
Warrenton NC, 27580
(Room 217 in the Department of Social Services Building)
Connect with Trillium
Get texts or emails and follow us on social media.
